In the intricate world of healthcare, revenue cycle management (RCM) stands as a vital pillar, ensuring healthcare providers receive timely and accurate payments for the services they render. The revenue cycle encompasses a series of interconnected stages, from patient registration to claim submission and payment collection. Effective Revenue cycle management in medical billing plays a pivotal role in maximizing revenue, minimizing errors, and maintaining financial stability for healthcare organizations. Beyond financial gains, RCM also impacts patient satisfaction and overall operational efficiency, making it a critical aspect of modern healthcare management.
The efficient management of the revenue cycle is essential for healthcare providers to ensure timely and accurate reimbursement, maximize revenue, and maintain financial stability. By navigating through the complexities of medical billing and minimizing errors, RCM plays a pivotal role in optimizing financial outcomes for healthcare organizations while upholding the highest standards of patient care and satisfaction.
Understanding the Revenue Cycle in Medical Billing
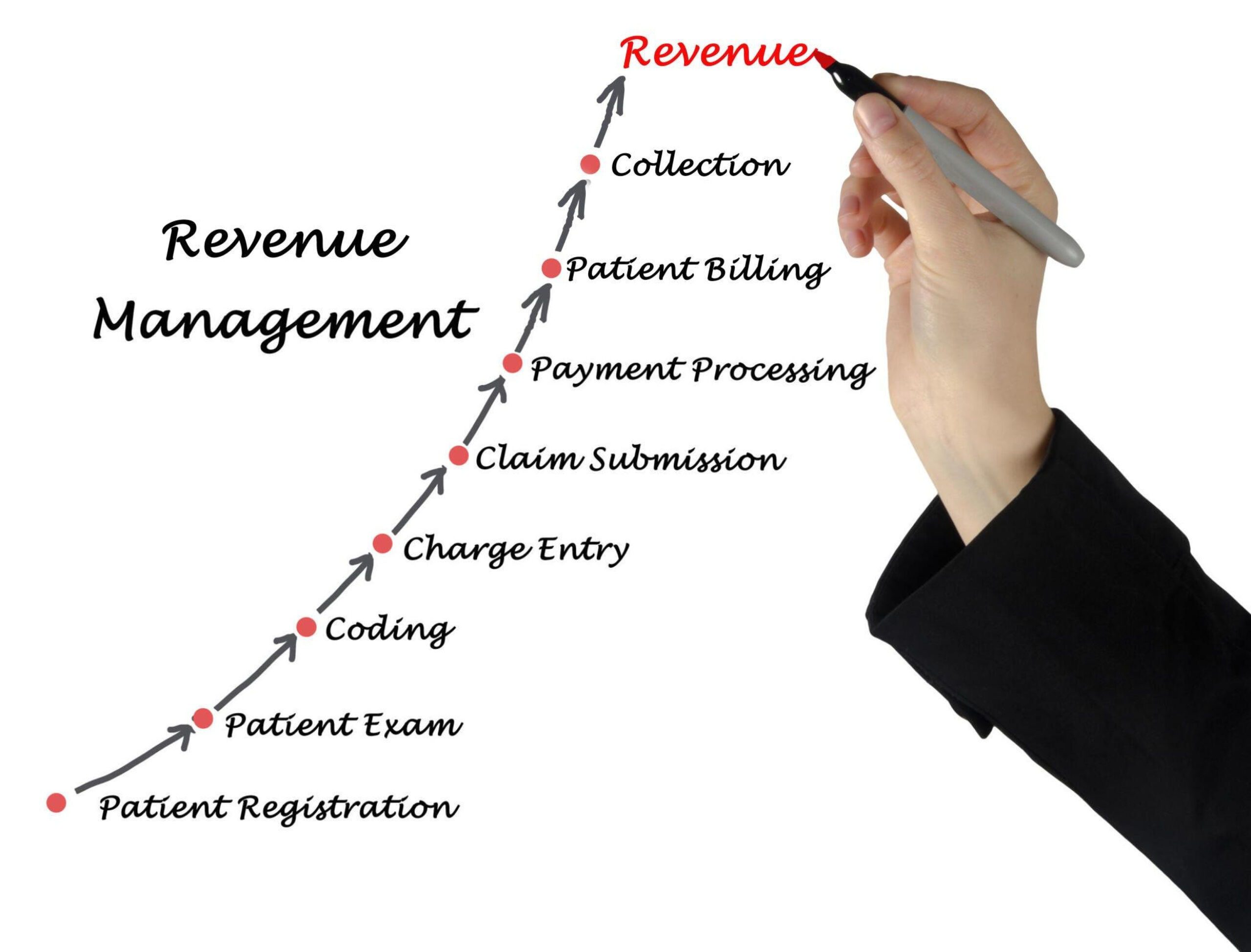
The revenue cycle in medical billing is a complex journey that commences with patient registration and concludes with successful payment collection. This intricate process involves several stages, including:
Patient Registration: The revenue cycle begins when patients provide their demographic and insurance information during the registration process. Accurate data collection at this stage lays the foundation for a smooth billing process.
Eligibility Verification: Before providing services, healthcare providers must verify a patient’s insurance coverage and benefits to ensure proper billing and reimbursement.
Coding and Documentation: Accurate medical coding and comprehensive documentation of services provided are critical to generating error-free claims.
Claims Submission: Completed claims are submitted to insurance payers for reimbursement. A thorough understanding of payer requirements and timely submission are essential for success.
Claims Adjudication: The insurance payer reviews the submitted claims and determines the amount of reimbursement, considering the patient’s insurance coverage and policy terms.
Payment Collection: After claims adjudication, healthcare providers receive payments from insurance payers, patients, or other third-party entities.
Denial Management: Handling claim denials and resubmissions is crucial to ensure that rightful reimbursement is obtained for the services rendered.
Maximizing Revenue through Effective Revenue Cycle Management
The optimization of the revenue cycle is vital for healthcare organizations to thrive financially. Here are key strategies that can enhance revenue generation:
Streamlined Billing Process: Implementing efficient billing workflows and utilizing electronic health record (EHR) systems can expedite the billing process, leading to quicker payment collection.
Comprehensive Eligibility Verification: Ensuring thorough eligibility verification before providing services helps avoid claim denials and reduces the risk of non-payment.
Charge Capture Accuracy: Capturing all services and procedures provided accurately is essential for proper billing and maximum reimbursement.
Timely Claims Submission: Prompt claims submission improves cash flow and reduces the risk of delayed payments.
Effective Denial Management: Proactive handling of claim denials, identifying the root causes, and resubmitting denied claims efficiently ensures full reimbursement for services provided.
Minimizing Errors in Revenue Cycle Management
Errors in the revenue cycle can result in payment delays, claim denials, and revenue loss. To minimize errors and ensure smooth revenue management, consider the following practices:
Ongoing Staff Training: Regular training programs for billing and coding staff keep them updated with the latest industry regulations and best practices, reducing errors.
Utilizing Technology: Investing in advanced RCM software and EHR systems streamlines processes and minimizes manual errors in claims submission and documentation.
Conducting Internal Audits: Regular internal audits of coding, billing, and documentation practices help identify and rectify errors before they affect revenue.
Monitoring Key Performance Indicators (KPIs): Tracking essential KPIs, such as denial rate and days in accounts receivable, enables healthcare organizations to identify areas for improvement.
Collaborating with Payers: Maintaining open communication with insurance payers can help resolve claim disputes and clarify billing requirements.
Conclusion
Efficient revenue cycle management is a cornerstone of financial stability and success for healthcare organizations. By streamlining billing processes, ensuring accurate documentation and coding, and implementing effective denial management strategies, healthcare providers can optimize their revenue cycle and enhance overall financial performance. Minimizing errors through regular training, leveraging technology, conducting internal audits, monitoring KPIs, and fostering collaboration with payers further strengthens the effectiveness of revenue cycle management in medical billing. In an ever-evolving healthcare landscape, staying abreast of industry regulations and implementing best practices is vital for successful revenue cycle management, empowering healthcare organizations to thrive financially while delivering exceptional patient care.








